โรคและการรักษา

Sudden Death คืออะไร? โปรแกรมตรวจคัดกรองความเสี่ยงภาวะเสียชีวิตกะทันหัน
Sudden Death: ภาวะที่อวัยวะสำคัญของร่างกายหยุดทำงานกะทันหัน เกิดขึ้นแบบเฉียบพลันและรุนแรง ส่งผลให้เสียชีวิตทันที หรือภายใน 1 ชั่วโมงหลังมีอาการ เกิดขึ้นได้กับทุกคน โดยแทบไม่พบสัญญาณเตือนล่วงหน้า

ตาพร่ามัว (Blurred Vision)
ตาพร่ามัว เป็นอาการที่หลายคนเคยประสบเมื่อมองเห็นไม่ชัดเจน มองภาพแล้วเบลอ เหมือนมีหมอกหรือฝ้ามาบังสายตา อาการนี้อาจเกิดขึ้นได้ทั้งในตาข้างเดียวหรือทั้งสองข้าง อาจเกิดชั่วคราวหรือเป็นระยะยาวได้

ปวดท้อง (Abdominal pain) ปวดท้องตรงไหน อาจบอกโรคอะไร
ปวดท้อง (Abdominal pain) คือ อาการปวดที่บริเวณใดบริเวณหนึ่งของท้อง หรือปวดทั่วบริเวณท้องระหว่างซี่โครงและกระดูกเชิงกราน อาการปวดท้องมีสาเหตุจากอวัยวะต่าง ๆ ภายในช่องท้อง

เหงื่อออกมือ สัญญาณบอกโรคอะไร อันตรายไหม
เหงื่อออกมือ อาจดูเหมือนเป็นเรื่องปกติสำหรับบางคน แต่การที่เหงื่อออกมือมากเกินไปอาจส่งผลต่อคุณภาพชีวิตและการเข้าสังคม จนไม่กล้าใช้มือหยิบจับสัมผัสหรือแม้แต่จับมือกับผู้อื่น

โรคหลงตัวเอง หรือ บุคลิกภาพแบบหลงตัวเอง (NPD)
โรคหลงตัวเอง หรือ บุคลิกภาพแบบหลงตัวเอง (NPD) เป็นปัญหาสุขภาพจิตที่พบในผู้ชายมากกว่าผู้หญิง มักแสวงหาความสนใจ ต้องการการยอมรับจากผู้อื่น มักขาดความเห็นอกเห็นใจ
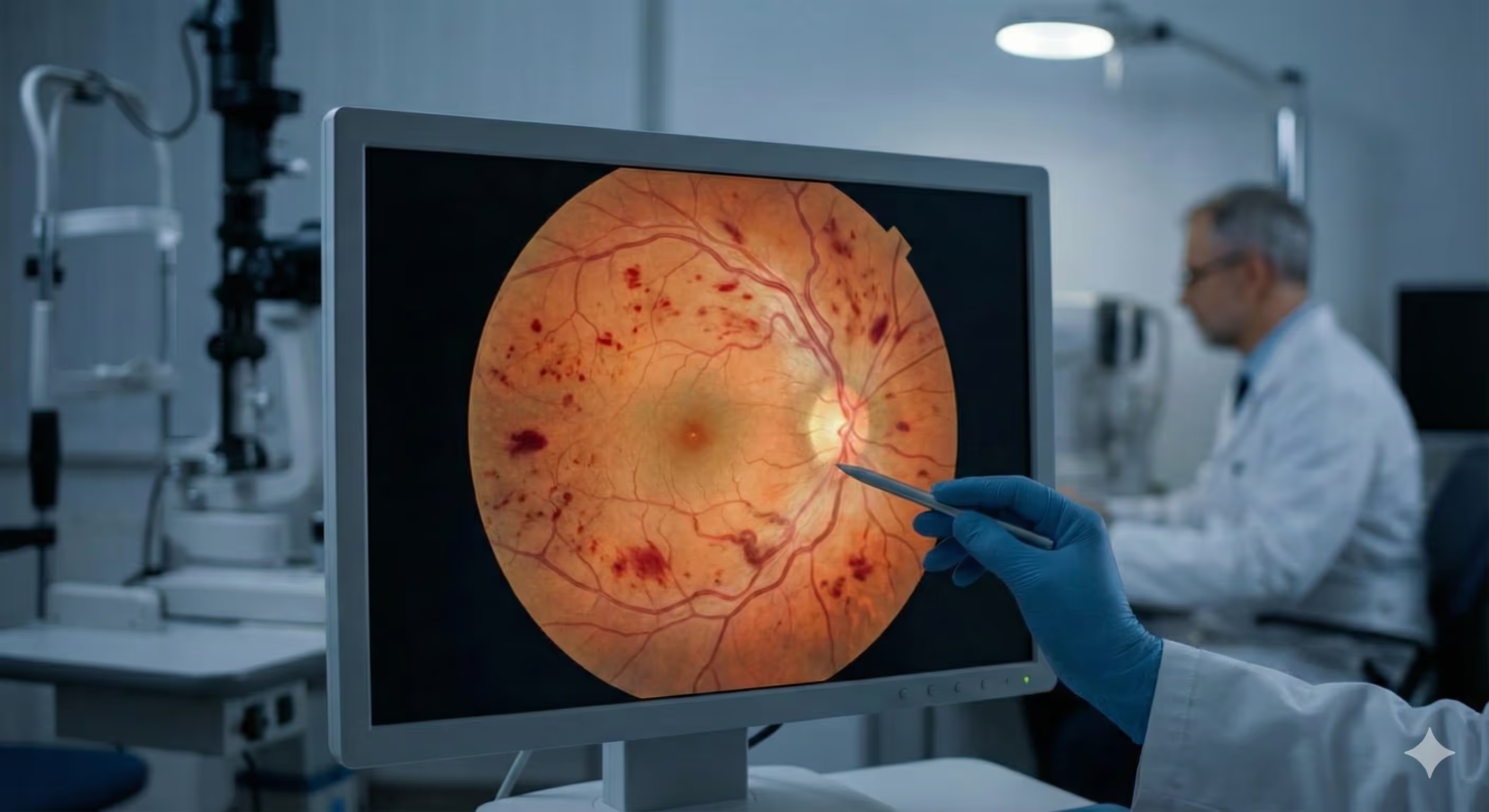
หลอดเลือดดำในจอประสาทตาอุดตัน (RVO)
หลอดเลือดดำในจอประสาทตาอุดตัน (Retinal Vein Occlusion) เป็นภาวะที่ส่งผลให้ตาพร่ามัว สูญเสียการมองเห็นอย่างเฉียบพลันและรุนแรง โดยมักส่งผลกระทบต่อดวงตาข้างเดียว

อาการปวดหัว จากลิ่มเลือดอุดตันหลอดเลือดดำในสมอง
ปวดหัว หรือ ปวดศีรษะ อาการสามัญประจำบ้านที่ไม่ว่าใครก็ต้องมีประสบการณ์ปวดกันมาบ้าง ไม่ว่าจะปวดมากปวดน้อย ปวดข้างเดียว ปวดเข้าเบ้าตา ปวดทั่วใบหน้า สารพัดปวด ซึ่งอาการเหล่านี้มีสาเหตุหลากหลาย

รักษามะเร็งตับ โดยการจี้ความร้อน RFA หรือ MWA ข้อบ่งชี้ ข้อดี
รักษามะเร็งตับ โดยการจี้ความร้อน (Ablation therapy for liver cancer) คือ วิธีรักษามะเร็งตับโดยการใช้เข็มความร้อนจากคลื่นวิทยุ (RFA) หรือคลื่นไมโครเวฟ (MWA) จี้ทำลายก้อนมะเร็งโดยตรงผ่านผิวหนัง
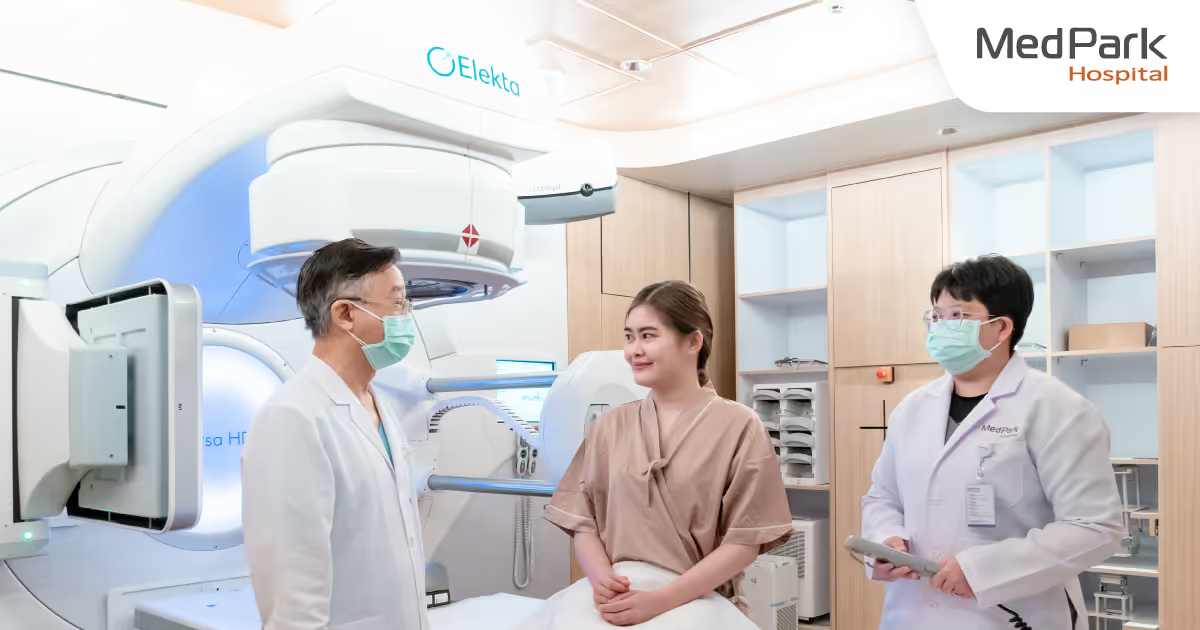
ฉายแสง มะเร็ง รังสีรักษา (Radiotherapy) กี่ครั้ง ขั้นตอน ผลข้างเคียง
ฉายแสง (Radiotherapy) หรือ รังสีรักษา คือ วิธีการรักษามะเร็งด้วยการฉายรังสีพลังงานสูง เช่น รังสีเอกซ์ แกมมา หรืออนุภาคประจุไฟฟ้าไปที่ก้อนมะเร็งเพื่อทำลายสารพันธุกรรม (DNA) ของเซลล์มะเร็งไม่ให้ แบ่งตัว